Common Dental Issues That Can Affect General Health

Understanding Common Dental Issues: Know How Your Mouth Dictates Your Body’s Health
We all know that the function of the mouth is to deliver essential nutrients inside the body. In this regard, maintaining oral health is important because poor oral hygiene can disrupt not only the teeth but also other body systems, including the digestive tract. Therefore, addressing common dental issues is vital to keep the oral-systemic connection working smoothly. Because oral health is closely linked to systemic health, many healthcare systems that provide primary care for adults and families also emphasize regular dental screenings as part of preventive care.
The purpose of your mouth is not just to flash bright smiles, but it is also the primary gateway to your respiratory and digestive tracts. When common dental problems in adults are not treated promptly, they become a reservoir for chronic inflammation. Not to forget, the bacteria that travel through the bloodstream to wreak havoc on your heart, brain, and beyond.
In this comprehensive guide, we explore these issues that act as silent killers, causing systemic diseases.
Most Common Dental Issues and Their Impact on Health
| Common Dental Issue | Main Cause | Symptoms | Potential Impact on General Health |
|---|---|---|---|
| Untreated Cavities (Dental Caries) | Bacteria in plaque converting sugars into acid that erodes enamel | Tooth pain, sensitivity to hot/cold foods, visible holes or dark spots | Infections, abscess formation, difficulty eating, nutritional decline, and possible spread of infection |
| Bruxism (Teeth Grinding) | Stress, sleep disorders such as sleep apnea, anxiety | Jaw pain, worn-down teeth, headaches, facial muscle tension | Temporomandibular joint (TMJ) disorders, chronic headaches, restricted jaw movement |
| Oral Cancer | Tobacco use, alcohol consumption, HPV infection, chronic irritation | Red or white patches, persistent mouth sores, difficulty swallowing | Cancer spread to lymph nodes, lungs, or liver if untreated |
| Gum Disease (Periodontal Disease) | Poor oral hygiene leading to bacterial plaque buildup | Bleeding gums, swelling, gum recession, loose teeth | Linked to cardiovascular disease, diabetes complications, and systemic inflammation |
While many oral conditions exist, three primary common dental problems in adults remain the dominant globally. These include the following:
Untreated Cavities (Dental Caries)
Cavities are the most common dental problems in adults. Significantly, these occur when bacteria in plaque convert dietary sugars into acid, which dissolves tooth enamel.
Impact on General Health
Beyond the risk of abscesses and sepsis, chronic tooth decay is one of the common dental issues where an individual faces productivity loss and nutritional decline. In addition, constant pain from cavities further leads to functional limitations, making it difficult to sleep, speak, or concentrate at work.
Bruxism (Teeth Grinding and Clenching)
Bruxism is also one of the ignored signs of poor oral health. Notably, it is a common physical response to stress or sleep disorders like sleep apnea. It involves the unconscious grinding or clenching of teeth, usually during sleep. Because chronic stress is a major trigger for this condition, improving access to accessible mental health care can also play an important role in managing the underlying causes of teeth grinding.
Impact on General Health
Bruxism leads to chronic headaches. Also, due to the constant pressure, the temporomandibular joint (TMJ) is damaged, leading to earaches and restricted jaw movement.
Oral Cancer
Another of the most common dental issues is oral cancer. Essentially, it is the 6th most common cancer worldwide. Because it often starts as a painless red or white patch, and is frequently caught too late.
Impact on General Health
Oral cancers affect both oral health and overall health. If not caught during a routine dental screening, oral cancer can quickly spread to the lymph nodes in the neck and eventually to the lungs or liver. Moreover, when a patient undergoes the treatment for oral cancer (radiation and chemotherapy), they often end up with Xerostomia (Dry Mouth).
Gum Disease and Its Link to Overall Health
Gum disease is one of the most common dental issues affecting general health. It may seem like a simple case of gingivitis, but if it gets worse the patient end up with red, swollen gums that bleed when you brush. Moreover, it can also progress to periodontitis, where the inner layer of the gum and bone pull away from the teeth and form pockets.
The Mechanism of Harm
Periodontal disease symptoms usually lead to chronic and inflammatory conditions. Moreover, when your gums are infected, they become “leaky.” This allows oral bacteria, such as Porphyromonas gingivalis, and inflammatory markers like C-reactive protein to enter your bloodstream. Once in circulation, they become prone to target the immune response throughout the body.
Associated General Health Risks
The following are the oral health and overall health risks that start to develop if periodontal issues are left untreated:
Cardiovascular Disease
When oral practices are compromised, bacteria from the mouth easily attach to fatty plaques in the bloodstream. Consequently, these contribute to the hardening of the arteries (atherosclerosis).
According to a published news report by the University of Copenhagen:
“Children with severe gum disease are up to 45% more likely to suffer from heart attacks or strokes as adults.”
Diabetes
Most adults often overlook the relationship between common dental issues and diabetes. It is important to know that chronic gum inflammation makes it harder for the body to use insulin, leading to higher blood sugar levels. Conversely, this increased sugar levels then feeds the bacteria that cause gum disease.
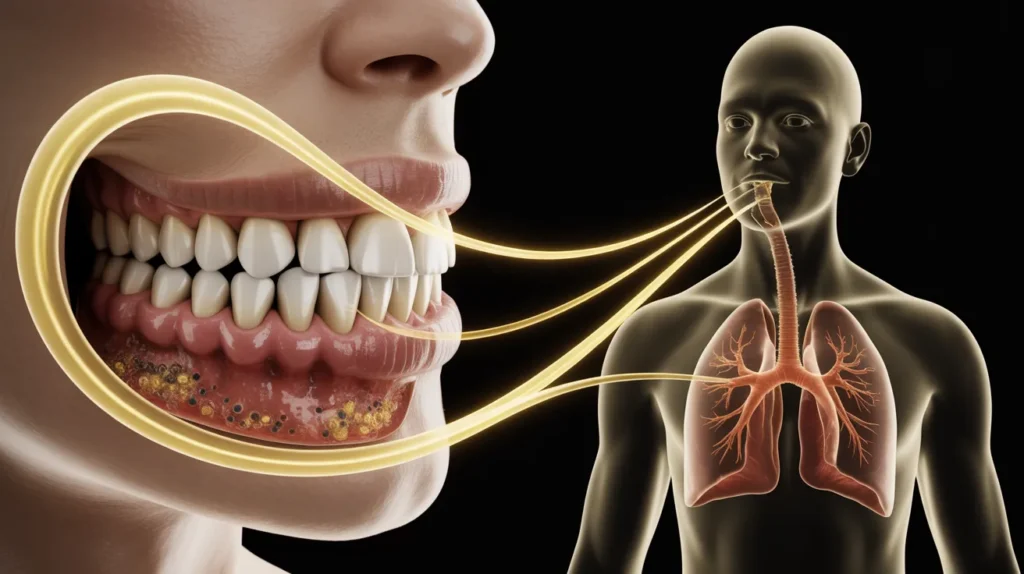
Respiratory Infections
When you inhale your bad breath, the oral bacteria enter your lungs, potentially ending up causing you pneumonia or aggravating Chronic Obstructive Pulmonary Disease (COPD).
Tooth Decay: One of the Most Common Dental Issues
Tooth decay is one of the most common dental problems globally. Whether a child or adult, many view a cavity as a minor issue, but it is important to know that if these cavities are left untreated, they can lead to a dental abscess. Not to mention, it is a pocket of pus caused by a bacterial infection.
The Underlying Damage
A dental infection doesn’t always stay in the tooth. The signs of poor oral health start to show up when the bacteria reach the pulp. Notably, it is the center of the tooth containing nerves and blood vessels.
- In severe cases, the infection leads to Ludwig’s Angina (a life-threatening skin infection under the tongue).
- Some cases also develop sepsis, where the body’s immune system overreacts to the infection and begins damaging its own organs.
Associated General Health Risks
The following are a few health risks associated with tooth decay:
Endocarditis
This is an infection which can cost you your life, as the inner lining of your heart chambers and valves starts to deteriorate. Typically, it occurs when bacteria from the mouth spread through the bloodstream and attach to damaged areas in the heart.
Nutritional Deficiencies
The periodontal disease symptoms of tooth decay result in painful cavities, requiring patients to opt for soft food diets. This malnutrition can weaken the immune system further.
How Oral Infections Can Affect the Body?
When bacteria form due to common dental issues, this results in a decayed tooth or infected gum pocket. Plus, this infection reaches your vital organs.
The Hematogenous Pathway (The Bloodstream)
This is the most direct route when your oral health and overall health is on stake. You must know that your gums are incredibly vascular (rich in blood vessels). When you have gum disease, the protective barrier of the skin inside your mouth breaks down.
Bacteremia
Simple activities like chewing or brushing can push bacteria into the bloodstream. Couple with that, if the bacterial infection is not looked after, these pathogens can hitch a ride to the heart, where they may attach to valves, or to the brain, where they can cross the blood-brain barrier.
The Respiratory Pathway (Aspiration)
When common dental issues team up with pathogenic bacteria, it can lead to decay or heavy tartar buildup.
Impact
This pathogenic bacterium results in the following:
- For elderly patients or those with weakened immune systems, this is a leading cause of aspiration pneumonia.
- Even in healthy individuals, it can exacerbate asthma and chronic bronchitis by keeping the airways in a state of constant irritation.
The Inflammatory Cytokine Signals
Sometimes, the periodontal disease symptoms make your immune system release pro-inflammatory cytokines. On top of this, these chemicals travel through the body, signaling other organs to go on high alert by making your cells resistant to insulin, directly contributing to Type 2 Diabetes and Metabolic Syndrome.
The Connection Between Oral Health and Heart Disease
The link between gum disease and heart disease is no longer a mere association, but it is a documented biological pathway. Clinically proven, people with moderate to severe gum disease have a 20% to 30% higher risk of developing heart disease.
Atherosclerosis (Hardening of the Arteries)
The most common dental issues often result in the buildup of plaque in the arteries.
The Hitchhiking Bacteria
According to prominent research, oral bacteria, such as Porphyromonas gingivalis, build inside the fatty deposits of human arteries.
The Mechanism
Once the bacteria finds its way through bleeding gums, they attach to the blood vessel walls. This triggers an immune response that causes the vessel walls to thicken and narrow, restricting blood flow and potentially leading to a heart attack or stroke.
Infective Endocarditis
Endocarditis is a rare gum disease and heart disease that can be life-threatening. It occurs when bacteria from the mouth spread through the blood and attach to damaged areas of the heart.
C-Reactive Protein (CRP) and Chronic Inflammation
Even if signs of poor oral health don’t physically reach the heart, the infection from your gums produces C-reactive protein (CRP). When the CRP levels turn high in the blood, the risk of cardiovascular diseases automatically increases.
How Diabetes and Gum Disease Are Related?
Diabetes and gum disease are closely related because of their bidirectional properties. This means that not only does diabetes make gum disease worse, but gum disease actually makes diabetes harder to control.
How Diabetes Affects Your Gums
Common dental issues that result in gum infections make diabetic patients sensitive to the following three primary health issues:
Thickening of Blood Vessels
Diabetes already thickens the blood vessels, and when gums are also affected, the body slows the efficiency of nutrient delivery and waste removal from the mouth tissues.
High Sugar in Saliva
When your blood sugar is high, the glucose levels in your saliva also rise.
Reduced Healing Power
Diabetes reduces white blood cells and weakens the defence system. Now, when a minor case of gingivitis is diagnosed in an individual, it will quickly spiral into bone loss for a person with diabetes.
How Gum Disease Affects Your Blood Sugar
Chronic gum disease acts as a continuous source of systemic inflammation. Therefore, the following health conditions easily develop:
Insulin Resistance
When your gums are infected, inflammatory chemicals like cytokines are released. These chemicals enter the bloodstream and interfere with the way your cells respond to insulin.
The HBA1c Connection
Clinical trials have shown that when patients with Type 2 diabetes receive a root canal to treat their gum disease, their HbA1c levels can drop by as much as 0.4% to 0.6%. In medical terms, that is often as effective as adding a second glucose-lowering medication.
Signs and Symptoms of Common Dental Issues
Several common dental issues develop silently until they reach an advanced stage. However, there are a few warning signs you should never ignore:
- If your gums bleed when brushing or flossing, it is a clear sign of infection developing.
- When a bad odour from your mouth remains persistent, know that there is bacterial buildup in periodontal pockets.
- Sharp pain when consuming hot or cold foods is a clear sign of dental sensitivity.
- Loose teeth are another prominent sign of bone loss and advanced periodontal disease.
- Gums appearing to move away from the tooth often start exposing the roots.
Risk Factors That Increase Dental Problems
While everyone should practice oral hygiene, some factors increase the risk of common dental problems in adults:
- Smoking is a primary risk factor for gum disease; it reduces blood flow to the gums, slowing down the healing process.
- A poor diet with increased amounts of processed sugars and refined carbohydrates feeds the bacteria that cause decay.
- Saliva is your mouth’s natural defense against acid. Medications, aging, or medical conditions that cause dry mouth leave teeth vulnerable.
- Chronic stress can lead to teeth grinding (bruxism) and a weakened immune system, making it harder to fight off oral infections.
Preventing Common Dental Issues Through Good Oral Hygiene
Prevention and timely intervention for common dental issues can save you from a silently growing health condition. Therefore, a medically approved oral hygiene routine includes:
Two-Minute Brushing
Opt for a fluoride toothpaste and brush at least twice daily.
Interdental Cleaning
Flossing or using interdental brushes must not be ignored. You must know that your toothbrush cannot reach the surfaces between your teeth.
Balanced Nutrition
Limiting sugary snacks and increasing intake of water, crisp vegetables, and calcium-rich foods.
Regular Screenings
Professional cleanings through regular dental visits remove tartar (hardened plaque) that home tools cannot.
When to See a Dentist for Common Dental Problems
Do not wait for pain to disrupt your routine, as it is often a late-stage signal that a dental structure has already been compromised. If you notice any of the following symptoms, schedule an appointment with a qualified Flower Mound family dentist, such as the team at Supreme Smiles Dentistry. In cases of sudden swelling, severe pain, or infection, seeking prompt care, similar to a same day sick visit in primary healthcare, can help prevent the condition from worsening.
- Any sudden change in the color or texture of your gums.
- A persistent metallic taste in your mouth.
- Any localized swelling in the gums, face, or neck.
- Sensitivity that lasts for more than a day or two.
Your oral health and overall health both are essentially connected. Therefore, by keeping your mouth healthy, you are also protecting your heart, your metabolism, and your long-term vitality.
In The End
Your mouth is the gateway through which your body gets the nutrition to function efficiently. Therefore, by timely addressing common dental issues, you are not just managing a simple cavity or a minor gum bleed but limiting the risk of any chronic disease. Furthermore, by prioritizing your oral hygiene today, you are protecting your heart, your brain, and your teeth.
Frequently Asked Questions (FAQs)
Q1. Can poor oral health actually cause a heart attack?
Yes, oral bacteria from infected gums can enter the bloodstream and contribute to the formation of arterial plaques. This further hardens and narrows your arteries, increasing the risk of cardiovascular events, including heart attacks and strokes.
Q2. If I don’t have any pain, why should I worry about my gums?
Periodontal disease symptoms are often painless in their early stages. Many people have active gum infection without realizing it until the disease has progressed to the point of bone loss or loose teeth. Therefore, regular professional cleanings are the only way for timely intervention.
Q3. How often should I see a dentist if I have diabetes?
While a standard patient may go every six months. However, many dentists recommend a three-month cleaning schedule for patients with diabetes to keep inflammation low and blood sugar management on track.
Q4. Is there a connection between oral health and pregnancy?
Yes, pregnancy causes hormonal fluctuations that increase the blood supply to gum tissues, making them more reactive to bacteria. If this leads to periodontitis, the inflammatory response can release chemicals that may trigger premature labor.
Q5. Why does my dentist ask about my heart medications?
Many heart medications cause Xerostomia (dry mouth) as a side effect. When your mouth is dry, your risk for cavities and infections skyrockets. At this point, your dentist can help you manage your oral environment and protect your teeth from the side effects of your life-saving medication.